I've written about perspective before, specifically how living with Jeff's spinal cord injury has opened up an entirely new perspective on life for us.
But I've recently experienced another new perspective that I wanted to share.
Last month, just ten days into the new year, I received news that I would put into the category of; "a caregiver's worst nightmare."
I was diagnosed with breast cancer.
Quite suddenly, I had become "sick." Of course I physically felt fine, but I was now aware that there were cells in my body that were not fine at all. And I would need surgery to remove them. And I would need time to recover. And I would need help.
All I could think about was how am I going to take care of Jeff when I need care myself?
The rest of January was a whirlwind of medical appointments for me followed by a couple weeks of waiting for pieces to fall into place. During the waiting period, I joined an online support group and walked a fine line between doing the right amount of research to educate myself while being cognizant of not going down the virtual rabbit hole of doom.
By the time I met with my surgeon in early February and knowing the tumor in my breast was on the larger side, I was prepared for her recommendation: mastectomy.
Of course it's not at all what I wanted to hear. I wanted her to say the tumor had magically disappeared, that I wouldn't need surgery afterall, and I could just go back to being my husband's caregiver and taking care of my family. But that didn't happen. Instead, she explained the surgery to me, told me what to expect physically afterward, and when I told her about my caregiving responsibilities, she told me that's something I would definitely need help with - for a few weeks at minimum.
When I got home, I shared the news with some close loved ones. And they all asked me the same question: how do you feel about this?
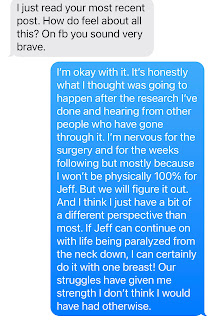
And as I wrote back to them, I found myself saying the same thing over and over - that the last decade of living with Jeff's injury has given me a different perspective than most. I explain it in a response to my dear friend Shannon who has given me permission to share (my comment is in blue):
Here's where I write about my perspective: ... I think I just have a bit of a different perspective than most. If Jeff can continue on with life being paralyzed from the neck down, I can certainly do it with one breast! Our struggles have given me strength I don't think I would have had otherwise.
But that's not the perspective this post is about.
Here's the rest of our conversation:
Shannon writes: I'm so proud to be your friend with what you've done with your life.
What?? Her words touched me deeply - and also completely caught me off guard.
What did she mean "what I've done with my life"? Because from my perspective it really seemed like life was the one doing stuff to me - not the other way around. I explained as much in my response:
I so often feel like I haven't done much or enough with life because it hasn't turned out the way I wanted or the way I planned. But your words are a reminder that life can still be meaningful and special even if it isn't the life you always wanted.
And then she dropped the REAL perspective:
What you do is endlessly meaningful because it impacts so many.
And just like that - bam - Shannon let me have a little glimpse of how others see me, see how I - how my family - has dealt with catastrophic challenges and how that's meant something to others.
She gave me a new perspective and reminded me that not just what I do, but how I do it, is important.
****
My surgery is scheduled for Friday, February 17th - one day after my 47th birthday. I never thought I'd be celebrating a birthday in my 40s by having my breast removed due to a cancerous tumor. But then again I also never thought my husband would be paralyzed just before his 40th birthday, and we would spend the next 10 years rearranging our life to accommodate his injury.
And I would be lying if I said I wasn't nervous. I am. Waves of anxiety wash over me as I think about the surgery, the cancer, the care, the treatment, the healing, the ... everything. There's a lot to think about and process.
So even though we don't have all the details worked out for Jeff's care after my surgery, we do have family who is willing to help, friends who have offered support, and a decade of hard core troubleshooting skills to draw strength from.
And of course that little thing called perspective that helps keep us going.